Welcome to Espire Dental in Encinitas, California!
Our beautiful Espire Dental Encinitas location, formerly named La Costa Dental Group, has been a beacon of dental excellence in the Encinitas community since 1975. A proud sponsor of youth sports throughout San Diego for over 50 years, our Espire Dental Encinitas team welcomes kids, teens and adults alike. The dentist is near the corner of El Camino Real and Grand View Road, we are just south of the Leo Mullen Sports Park.
At Espire Dental, our skilled dentists are here to create a healthy and well-deserved smile, with you in mind! We offer a wide range of comprehensive services, from preventative care, to restorative dentistry like crowns and bridges, and even wisdom teeth removal and implant placement. If you’re looking for a whiter, brighter and straighter smile, we’ve got you covered! Our providers are highly trained in Invisalign and teeth whitening, as well!
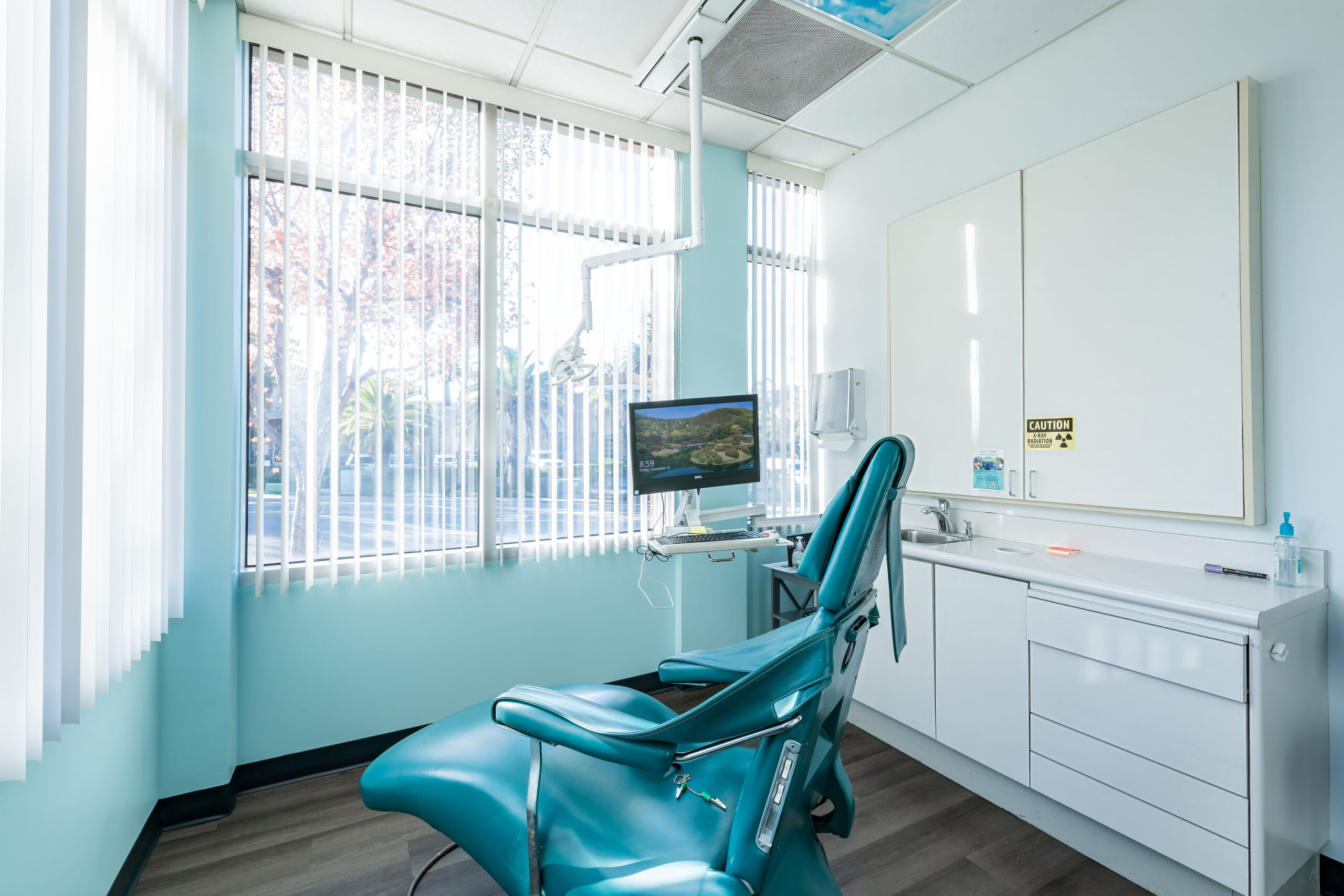
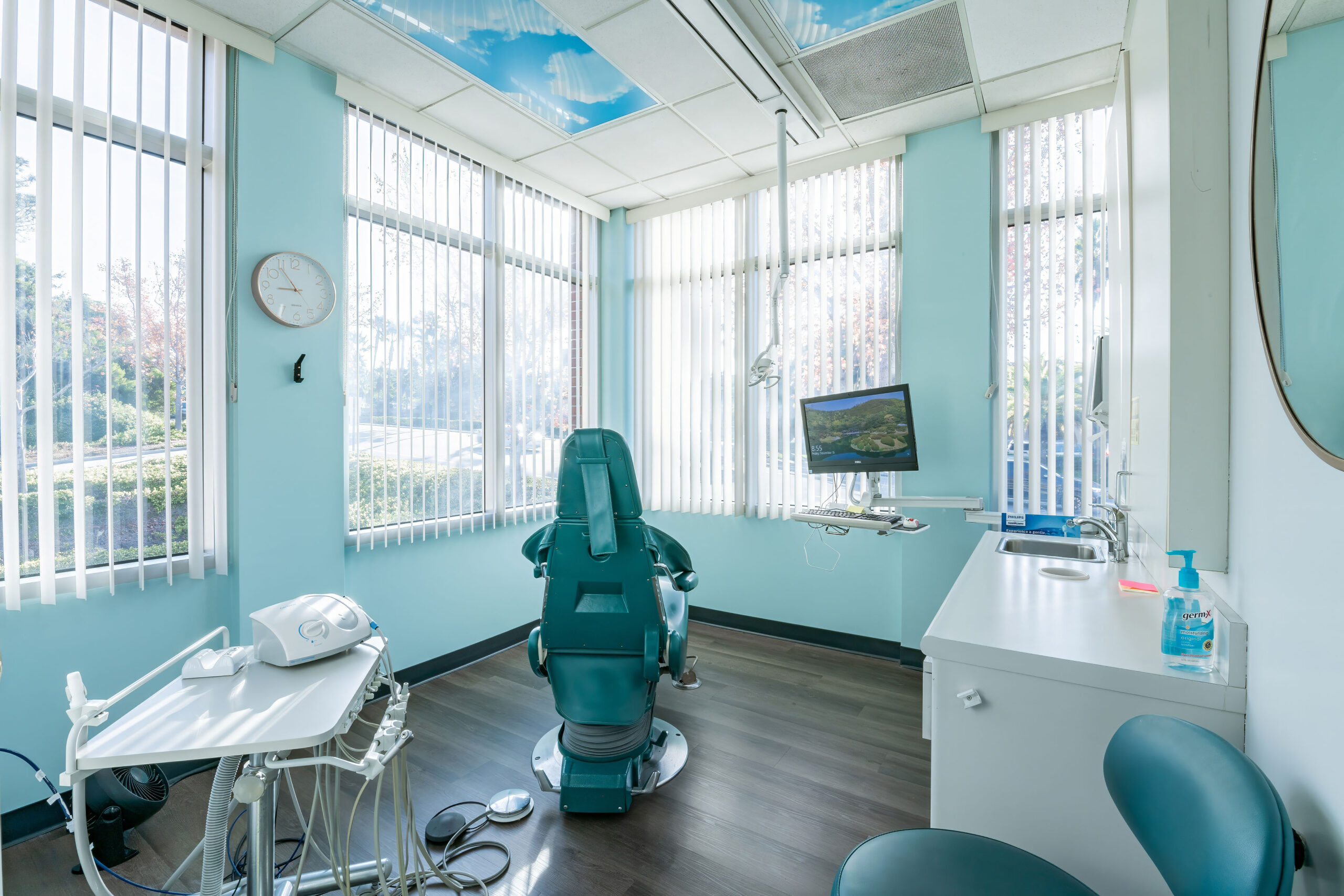
We pride ourselves on being your dental one-stop-shop, and promise to provide you with the excellent dental care you deserve. We combine modern technology, like digital x-rays and intraoral imaging, to patient amenities for comfort and ease. Noise-canceling headphones – check. Cozy blanket for warmth – yes please. Neck pillow for ultimate comfort – absolutely! We welcome you to visit us at Espire Dental in Encinitas, and enjoy a dental experience unlike any you’ve ever had!
We invite you to join our dental family and experience the Espire difference for yourself. Our passionate team is excited to help you achieve the healthy, beautiful smile you deserve. Contact us today to schedule your appointment and embark on a journey to optimal oral health. Together, we’ll make your smile shine brighter than ever!




 General Dentistry
General Dentistry